4.09 Health and Social care interface
Presented by:
Dr Iain Wilkinson (Consultant Geriatrician East Surrey Hospital)
Dr Jo Preston (Consultant Geriatrician St George’s Hospital)
Faculty: Jackie Lelkes and Wendy Grovesner, Tracy Szekely
Broadcast date: 5th December 2017
Sip of MDTea

CPD log
Click here to log your CPD online and receive a copy by email.
Tweetchat #MDTeaClub
We will be hosting a ‘journal club’ type tweet chat to discuss topics raised in this episode using #MDTeaClub
Join us to discuss topics raised in the episode and spread any resources you may have!
Show Notes
Learning Outcomes
Knowledge:
- To understand what integrated care is
- To understand how greater collaborative working between health and social care is beneficial
- To consider some models of integrated care
Skills:
- To gain a better understanding of the concept of and benefits of integrated care
- To understand the history of the development of integrated care
- To consider some of the difficulties with this approach to care.
Attitudes:
- To understand the importance of health and social care working constructively together for the benefits of the patient/service user
- To understand the benefits to the whole system of an integrated approach to care and support for older people
Interface between health and social care
Big questions in the NHS and adult social care are:
- How can they be integrated so as to serve people better and save money at the same time?
- Between 2011-12 and 2015-16 spending by NHS trusts and NHS foundation trusts increased by 11%,
- Local authority spending on adult social care has reduced by 10% since 2009-10.
- Key measures of the performance of health and social care sectors are worsening.
- For example, between November 2014 and November 2016, delays in discharging patients from hospital increased by 37%, due to unavailability of social care and nursing home placements.
A survey by the Association of Directors of Adult Social Services (ADASS) and the NHS Confederation found that:
- 46% of respondents said that integrated care had improved quality of life for people with long-term conditions,
- 41% said they had been assisted to live more independently, and
- 48% said it had resulted in financial savings.
- There was a reductions of 15 – 20% of people going into residential/nursing home placements; and
- 20 – 30% in A&E attendance and hospital bed occupancy are achievable among people deemed to be at “high risk” of going into these forms of care.
Definitions:
What is integrated care?
Integration is about placing individuals at the centre of the design and delivery of care with the aim of improving a person’s outcomes, satisfaction and value for money.
Currently a plethora of definitions, which makes it difficult to set a clear pathway
Armitage, Suter, Oelke and Adair (2009) conducted a literature review and reported that more than 70 terms and phrases related to integration.
Robertson (2011) describes integrated care as being used to refer to:
- Health and social services delivered by a single organisation;
- Joint delivery of health and social care by more than one organisation
- Links between primary and secondary health care;
- Joining care at different levels within a single sector e.g. mental health services;
- Joining prevention and treatment services.
Practical Definition
National Voices, a coalition of health and care charities provide a definition of integrated care – embedded in the ‘Shared Commitment’ framework. A person-centred ‘narrative’ –
“I can plan my care with people who work together to understand me and my carer(s), allow me control, and bring together services to achieve the outcomes important to me”
Why look for integration?
The arguments for better integration are many including:
- In its fourth annual State of Care report, the Care Quality Commission suggested that at least 530,000 emergency admissions of older people to hospital in 2012–13 could have been prevented through better management of their conditions in the community.
- Shown to reduce unplanned admissions and delayed discharge while helping people to live independently for longer;
- There is a tendency to focus on the physical and practical aspects of rehabilitation rather than the social and emotional aspects of care, which are equally as important.
- GPs are finding that social workers are able to produce more subtle, less expensive solutions to people’s needs than the high-cost care they have often been given;
The recent focus on the integration of health and social care, and its potential to provide better, more cost-effective services, is in direct response to three pressing issues:
The drive to integrate health and social care is due to four main issues:
- An ageing population and shifts in the pattern of disease means that people are living longer with a mixture of needs
- By 2018 the number of people with three or more long-term conditions is expected to rise to 2.9 million, an increase of 50%, and if the care system is unreformed the additional cost will be £5 billion.
- The fragmentation and complexity in how services are commissioned funded and provided.
- Since the foundation of the NHS in 1948, responsibility for ‘social care’ has rested with 152 local authorities. Successive reorganisations have created new divisions
- The enactment of the NHS and Community Care Act 1990, lead to 90% of publicly funded social care services – such as care at home and residential and nursing home – being provided by private and voluntary providers.
- The Health and Social Care Act 2012 means that different parts of the NHS and care system – primary care, social care, acute hospitals, mental health and community health services – are commissioned and funded separately and subject to different governance, accountability and regulatory regimes.
- The longstanding distinction between NHS care that is mostly free at the point of use and funded through general taxation and publicly funded social care which is subject to a financial assessment – a ‘means test’.
- Spending cuts and a need to deliver further efficiency savings.
Lamb, N. (2013) Improving care through a joined up approach. Available at:
www. gov.uk/government/speeches/norman-lamb- improvingcare-through-a-joined-up-approach
The King’s Fund’s influential report, Where next for the NHS reforms? The case for integrated care argues that resources have to be used much more efficiently to meet the needs of an ageing population.
A new model of integrated care, it said, “would focus much more on preventing ill-health, supporting self-care, enhancing primary care, providing care in people’s homes and the community, and increasing coordination between primary care teams and specialists and between health and social care.”
Where next for the NHS reforms?
Why the divide?
In 1968, the Ministry of Health was dissolved and its functions transferred (along with those of the similarly dissolved Ministry of Social Security) to the newly created Department of Health and Social Security (DHSS). Twenty years later, these functions were split back into two government departments, forming the Department of Social Security (DSS) and the current Department of Health.
The cultural and physical divide between health and social care can often get in the way and NHS and social care professionals regularly fail to understand each other’s unique role, responsibilities and perspectives.
These barriers can be broken down with::
- Inter-professional education;
- Co-location; and
- Informal networking,
Integration can overcome the Organisational; Professional; and Legal and regulatory boundaries within the health and social care sectors
Most people would like a seamless service between health and social care, which ignores boundaries
People who use services and carers value services that are:
- Appropriate to their needs – they are less concerned with how these are organised.
- Timely assessment and services;
- Partnership and the development of trusting relationships with named key workers; and
- Improved communication and coordination between the agencies.
Better Care Fund
The Government’s principal policy to achieve integration is the Better Care Fund, £3.8b (not new money) described as ‘a single pooled budget for health and social care services to work more closely together’ so that older and disabled people are offered better, more integrated care and support.
The Better Care Fund has been successful in incentivising local areas to work together; more than 90% of local areas agreed or strongly agreed that delivery of their plan had improved joint working. There are report of improvements at the national level in reducing permanent admissions of people aged 65 and over to residential and nursing care homes, and in increasing the proportion of older people still at home 91 days after discharge from hospital into reablement or rehabilitation services.
So why is integration difficult?
The barriers to integrated care for people with long-term conditions have been identified by a wide range of reports and reviews, and include:
- Single condition services: services dealing with single conditions, with attendant dangers of polypharmacy, and excluding a holistic approach to service users.
- Lack of care coordination: people being unaware of whom to approach when they have a problem, and nobody having a generalist’s ‘bird’s eye’ view of the total care and support needs of an individual.
- Emotional and psychological support: in particular, a lack of attention to the mental health and wellbeing of people with ‘physical’ health problems.
- Fragmented care: the healthcare system remaining within its own economy, and not being considered in a whole system approach with social care or other services important to people with long term conditions (e.g. transport, employment, benefits, housing).
- Lack of informational continuity: care records which can’t be accessed between settings, or to which patients themselves don’t have access.
- Reactive services, not predictive services: failure to identify vulnerable people who might then be given extra help to avoid hospital admission or deterioration/complications of their condition(s).
- Lack of care planning consultation: services which treat people as passive recipients of care rather than encouraging self-care and recognising the person as the expert on how his/her condition affects their life.
Some additional barriers to integrated care are more substantial, based on how the NHS and social care has been constructed:
- England has legally distinct health and social care systems.
- The NHS is free at the point of use, while local authorities typically only pay for individual packages of care for adults assessed as having high needs and limited means.
- Both systems are made up of a complex range of organisations, professionals and services.
Local areas can choose to integrate services in a broad range of ways and how they do so depends on the needs of the local population, and on existing care services and structures. Integration is not about organisations merging and can cover a range of types of cooperation. For example:
- At patient/service use level: local areas can introduce joint assessments of a person’s care needs across more than one service and involving more than one care professional;
- At service level: local areas can bring together several services into one place for people with a single condition, such as diabetes; and
- At organisational level: local areas can pool budgets or jointly commission services i.e. intermediate care
Current Policy drivers:
- In 2013, the Department of Health launched the five-year Integrated Care and Support Pioneers Programme to support its commitment for “urgent and sustained action” to make joined-up and coordinated health and care the norm by 2018.
- 25 integrated care pioneer sites (the pioneers) are developing and testing new and different ways of joining up health and social care services across England, utilising the expertise of the voluntary and community sector, with the aim of improving care, quality and effectiveness of services being provided.
- In 2014, NHS England published its Five Year Forward View, setting out how it aims to achieve a financially sustainable health and care system by 2020 including through integration.
- The government reiterated its commitment to joining up health and social care in the Spending Review and Autumn Statement 2015. It delayed until 2020 its target date for health and social care to be integrated across England, with local areas required to produce a plan by April 2017 for how they would achieve this
- However the National Audit Office warns that progress with integration of health and social care has, to date, been slower and less successful than envisaged and has not delivered all of the expected benefits for patients, the NHS or local authorities. As a result, the government’s plan for integrated health and social care services across England by 2020 is at significant risk. (Audit Commission, 2016)
- Unfortunately the integration of health and social care services has been piecemeal and individually programme based, with good examples tending to be the exception rather than the rule. There is wide variation, inconsistencies in policy and project implementation, and often no significant learning mechanisms in place to aid the transference of best practice (RCN, 2011).
Organisational
| Enablers | Barriers | ||||
education and Training
|
|
People and relationships
| Enablers | Barriers | ||||
|
|
Financial
| Enablers | Barriers | ||||
|
|
Policy
| Enablers | Barriers | ||||
|
|
(Sources: NHS Future Forum, 2012; Goodwin et al, 2012; Rand Europe and Ernst and Young, 2012; National Leadership and Innovation Agency for Healthcare, 2011; Cameron et al, 2012; Suter et al 2009).
How it can work: A case study
(FromA report by The College of Social Work and the Royal College of General Practitioners (2014) .)
Jill is 80 and lives alone. She has chronic obstructive pulmonary disease, arthritis and high blood pressure. Jill’s family live nearby, they are working and help her when they can. Jill gets out once a week to a lunch club but struggles with walking or standing. She is scared of falling but wants to remain in her own home.
What integrated care means for Jill
- Better coordination of care with a single point of contact (keyworker) for her and her family.
- One concise, integrated care plan that addresses all her needs and informs her and her family what to do if she is unwell;
- Less duplication of assessment and less need to repeat information;
- More community-based support helping to reduce the need for hospital admissions;
- Assistance to learn about her conditions and how she can manage her health with the aim of remaining well and living more independently;
- More joined up service and greater continuity of care;
- More advice and support for her family who are providing care and support.
What it means for professionals
- Better joint working and greater understanding of each other’s roles, leading to the developments of skills and knowledge;
- Shared knowledge and ownership of issues;
- Greater awareness of resources, enabling more effective choice;
- Greater shared risk management;
- More creative responses to need, particularly important with reduced funding;
- Increased focus on prevention and less reliance on formal support, greater use of the voluntary and third sector and informal support networks;
- Fewer avoidable hospital admissions, A&E attendances and care home admissions.
- Faster access to all relevant information;
- A proactive rather than reactive service;
- Mechanisms for integrated team working, so that no one should fall down the gaps in the service;
- Breaking down barriers between services, making life easier for patients/service users.
GPs and Social Workers: Partners for Better Care Delivering health and social care integration together .A report by The College of Social Work and the Royal College of General Practitioners (2014)
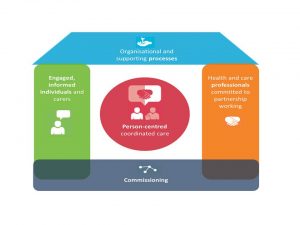
A solution: The House of care: An approach to integrated care:
NHS England and partners are using the ‘House of Care’ model as a checklist/metaphor for these building blocks of high quality person-centred coordinated care. The House relies on four key interdependent components, all of which must be present for the goal, person-centred coordinated care, to be realised:
- Commissioning – which is not simply procurement but a system improvement process, the outcomes of each cycle informing the next one, with respects to the services to be commissioned.
- Engaged, informed individuals and carers – enabling individuals to self-manage and know how to access the services they need when and where they need them.
- Organisational and clinical processes – structured around the needs of patients and carers using the best evidence available, co-designed with service users where possible.
- Health and care professionals working in partnership – listening, supporting, and collaborating for continuity of care.
The House of Care model is useful for drawing together the building blocks of integrated care to include the essential elements of continuity:
- Informational continuity: by which people and their families/carers have access to information about their conditions and how to access services; health and social care professionals will have the right information and records needed to provide the right care at the right time.
- Management continuity: a coherent approach to the management of person’s condition(s) and care; which spans different services, achieved through people and providers collaborating in drawing up collaborative care plans.
- Relational continuity: having a consistent relationship between a person, family, and carers and one or more providers over time (and providers having consistent relationships with each other), so that people are able to turn to known individuals to coordinate their care.
There are at least three levels at which the House of Care framework can be used:
Personal level: gives professionals on the front line a framework for what they need to do along with the people for whom they provide care and other providers, and ask local commissioners to secure for them particular services.
Local/community level: a ‘whole system’ approach to provision of services, including ‘more than medicine’ offers (community links with social care, housing, transport, employment etc). This will need commissioners to decide on:
- What: What are the principles and philosophy behind the care which commissioners wish to provide e.g. National Voices ‘I’ statements and what is the model to use as a framework for providing this care for the overall population?
- Which: Which populations of people with LTCs require a customised House of Care approach due to their particular care needs, and how will they be identified (e.g. risk stratification approaches, GP disease register, frailty index etc)
- Where, When, and Whom: Decide the local model of care i.e. where and when will all the components of the house be delivered for each group of people, and by whom.
- How: Write the specification of how to achieve this including the financial model that will support what needs to be done (tariffs, contracts, incentives etc that match the model of care).
National level: what can national organisations such as NHS England and its partners do to enable construction of the House of Care at the community and personal levels).
Personalised care planning is at the centre of the house. A collaborative process designed to:
- Bring together the perspectives and expertise of both the individual and the professional(s) involved in providing care,
- Offering tailored personal support to develop the confidence and competence needed for effective self-management.
The side-walls of the house:
- Engaged, informed patients and health care professionals committed to partnership working.
- Need to consider that patients/service users may need extra encouragement to participate in a more active way than they are used to;
- Staff need to understand this new way of working,
- Value the contribution that each person can bring to their care and
- Develop the skills to support self-management.
- Partnership working also extends to colleagues, as care for people with long-term conditions will increasingly be provided by multidisciplinary teams, both within general practice but also linking with wider community, social care and specialist staff.
The roof of the house represents the robust organisational systems that are essential to ensure efficient processes, including:
- Reliable systems for identifying and contacting patients with long-term conditions;
- Flexible appointment systems that support linked contacts; and
- Allow for longer consultations when necessary; and
- Record systems that can be used to document and share care plans, and for monitoring outcomes.
An integrated approach to the provision of care and support – House of Care
Curriculum Mapping:
This episode covers the following areas (n.b not all areas are covered in detail in this single episode):
| Curriculum | Area | |
| NHS Knowledge Skills Framework | Suitable to support staff at the following levels:
| |
| Foundation curriculum | Section
3.11 | Title
Discharge Planning |
| Core Medical Training | Team working and patient safety
Communication with colleagues and cooperation Management and NHS structure | |
| GPVTS program | Section 2.03 The GP in the Wider Professional Environment
Section 3.05 Care of Older People
| |
| Geriatric Medicine – Higher specialist training | 3.2.6 Planning Transfers of Care and Ongoing Care Outside Hospital
50. Intermediate Care and Community Practice |