Episode 3.01 – Multimorbidity
In this episode we will be talking through the NICE guidelines for multimorbidity management – which are here
Presented by:
Dr Iain Wilkinson (Consultant Geriatrician East Surrey Hospital)
Dr Jo Preston (Consultant Geriatrician St George’s Hospital)
Mairead O’Malley (Specialty Pharmacist Brighton and Sussex University Hospital)
Broadcast date: 14th February 2017
Here is a sip of this week’s MDTea
CPD log
Click here to log your CPD online and receive a copy by email.
Episode 3.01 Multimorbidity – Show Notes
Download the show notes here
Learning Outcomes
Knowledge
- To understand the difference between frailty, multimorbidity and disability.
- To be able to explore the management principles of multimorbidity as set out in the NICE 2016 guidelines.
Skills
- To identify when a patient needs management specifically for their multimorbidity – as opposed to condition specific management.
Attitudes
- To appreciate that a person-centred approach is required when dealing with multimorbidity.
Key points from discussion
Case study: Mrs A
A 78 year old woman with previous MI, type 2 diabetes, osteoarthritis, COPD and depression.
Our hypothetical patient with 5 common mild to moderate diseases would be:
- Prescribed at least 11 medications with potentially up to 10 more
- Advised to routinely engage in 9 self care / lifestyle alterations
- Expected to attend 8–10 routine primary care appointments for her physical conditions
- Attend 4–6 GP appointments for her mental health appointments and should be offered somewhere between 8–30 psychosocial intervention appointments for things like: depression, smoking cessation support and pulmonary rehabilitation.
The Challenges of Applying UK Clinical Guidelines to People With Multimorbidity
Definition of multimorbidity
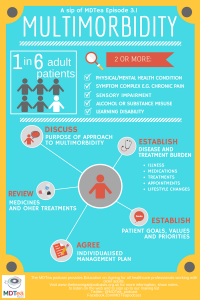
Be aware that multimorbidity refers to the presence of 2 or more long-term health conditions, which can include:
- Defined physical and mental health conditions such as diabetes or schizophrenia
- Ongoing conditions such as learning disability
- Symptom complexes such as frailty or chronic pain
- Sensory impairment such as sight or hearing loss
- Alcohol and substance misuse
Key point: be aware that frailty is not the same as multimorbidity, although there may be overlap
Nice guidance on multimorbidity ng56
NICE guidance
The paper itself is split into a few sections
- Recognising multimorbidity
- What to do about it (e.g. polypharmacy as main example)
- Recommendations for implementation (not covered in this episode)
Polypharmacy and multimorbidity assessments are one of the most challenging aspects of caring for older patients.
- For decades, single disease assessment and guidance were issued and accepted as best therapeutics and evidence based medicine.
- However, it has become apparent that with increasing complexity comes increasingly more difficult drug regimens and subsequent side effects.
- There have been lots of papers written on inappropriate medicines in elderly patients e.g. de Beers, PRISCUS criteria, PIDE tables etc.
Polypharmacy is not always a bad thing, in fact there are patients who are more than happy to take 20+ medicines to keep them well. However, there are others that are unhappy taking just 3. The fact of the matter is that it is and should always be the patient’s choice.
Polypharmacy can be defined as:
Appropriate: when
(a) all drugs are prescribed for the purpose of achieving specific therapeutic objectives that have been agreed with the patient;
(b) therapeutic objectives are actually being achieved or there is a reasonable chance they will be achieved in the future;
(c) drug therapy has been optimised to minimise the risk of ADRs and (d) the patient is motivated and able to take all medicines as intended.
Problematic: when one or more drugs are prescribed that are not or no longer needed, either because:
(a) there is no evidence based indication, the indication has expired or the dose is unnecessarily high;
(b) one or more medicines fail to achieve the therapeutic objectives they are intended to achieve;
(c) one, or the combination of several drugs cause unacceptable adverse drug reactions (ADRs), or put the patient at an unacceptably high risk of such ADRs, or because (d) the patient is not willing or able to take one or more medicines as intended.
NHS Wales medication review process:
- Is there a valid indication for this drug?
- Is this drug replacing a vital hormone e.g. thyroxine/insulin?
- Is this drug important in preventing rapid symptomatic deterioration e.g. PD meds?
- Is this drug providing day to day symptomatic benefit e.g. pain relief?
If the answer is yes to any of those questions then the drug should be continued…..if no then we should consider discussing with the patient reducing or stopping the treatment.
Resources
Polypharmacy – Guidance for Prescribing in Frail Adults
SIGN polypharmacy guidance (also available as an app)
Polypharmacy guidance Scotland 2015 – pdf
If you have some links or resources you’d like to share, get in touch and we’ll add them here.
Twitter @MDTea_podcast
Facebook www.facebook.com/MDTea
or email thehearingaidpodcasts@gmail.com
Curriculum Mapping
| Curriculum | Area |
| NHS Knowledge Skills Framework | Suitable to support staff at the following levels:
Personal and people development level 1-3 Service improvement level 1 |
| Foundation Curriculum 2012 | 2.1 Treats patient as centre of care
6.1 Lifelong learning 6.2 Evidence and guidelines 7.5 Safe prescribing 10.1 Manages patients with long term conditions 10.2 Supporting patient decision making |
| Foundation Curriculum 2016 | 2. Patient centred care
4. Self-directed learning 6. Interface with other healthcare professionals 10. Recognises, assesses and manages patients with long term conditions – Management of long term conditions in the acutely unwell patient – Support for patients with long term conditions 13. Prescribes safely – Clinically effective prescription – Discussion of medication with patients – Guidance on prescription – Review of prescriptions |
| Core Medical Training | Common competences:
System specific competences:
|
| GPVTS program | Section 2.03 The GP in the Wider Professional Environment
Section 3.01 – Healthy people: promoting health and preventing disease
Section 3.05 – Managing older adults
|
| ANP
(Draws from KSF) |
Section 13 Therapeutics and safe prescribing
Section 19. Managing long term conditions and promoting patient self-care Section 20. The patient as central focus of care |





1 Response
[…] in our episodes on multimorbidity and polypharmacy we saw that being treated by multiple specialist teams for multiple conditions […]