9.06 Music and Dementia
Presented by: Iain Wilkinson, Jo Preston, Alice O’Connor, Grace Meadows (Music therapist and programme director, Music for Dementia 2020)
Additional Guests: Jo White (Programme director, Wishing Well Music for Health), Dr Shreena Unadkat (clinical psychologist)
Broadcast date: 14th April 2020

Social Media
Jo: Lindsay Sanders @lindzOT has developed a simplified frailty scoring flow chart:
Learning Outcomes
Knowledge
- To be aware of current theories around musical memory and why it is important in dementia.
- To be aware of current evidence for the benefits of music in dementia.
- To understand what music therapy involves.
- To know where to find information about local music activities and experiences for people with dementia.
Skills
- To consider how using music in your own practice might help someone with dementia.
- To encourage communication with people who have dementia, or their caregivers, to find out about their interests and personal tastes in order to facilitate individualised care planning.
Attitudes
- To recognise pleasurable and social activities as an important part of a care plan.
- To promote the use of music in dementia and signpost others to sources of information about existing programmes and activities.
- To appreciate the role of the arts in dementia outcomes, and the link between this and socioeconomic inequality.
CPD Log
Show Notes
Definition
Oxford dictionary definition of Music as a mass noun:
Vocal or instrumental sounds (or both) combined in such a way as to produce beauty of form, harmony, and expression of emotion.
Origin: Middle English, from Old French musique, via Latin from Greek mousikē ‘(art) of the Muses’
https://www.lexico.com/definition/music
Main Discussion
Why music and dementia?
- Listening to music has a positive impact on mood and reduces stress.
- Music, memory and emotion are tightly interwoven, and music often triggers emotional memories (childhood holidays, leaving home, falling in love, births, deaths…) which are less likely to be affected by dementia.
- Nowadays, for better or for worse, music doesn’t cost much to listen to and it’s easily accessible.
- There is some evidence to suggest that music can improve the behavioural and psychological symptoms of dementia (BPSD) such as depression, agitation and aggression.
Effects of music on agitation in dementia: a meta-analysis
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5432607/
NICE guidelines 2015 for Older People, Independence and Mental Wellbeing:
Recommend group activities for people living with dementia “including singing programmes and choirs led by professional qualified people”.
https://www.nice.org.uk/guidance/ng32
NICE guidelines 2018 for Dementia:
Point towards ways in which music can be helpful, thanks to its inherent flexibility to support personalised care.
For example, “for people living with dementia who experience agitation or aggression, offer personalised activities to promote engagement, pleasure and interest.”
https://www.nice.org.uk/guidance/ng97
NERD ALERT
Music engages auditory, visual and motor regions of the brain.

Image: https://www.playlistforlife.org.uk/
The regions of the brain proposed to be responsible for musical memory are the anterior cingulate gyrus and pre-supplementary motor area.
This has been identified using functional MRI scanning of brain responses to pieces of music that were either new, recently heard or well known to participants.
https://www.ncbi.nlm.nih.gov/pubmed/26041611
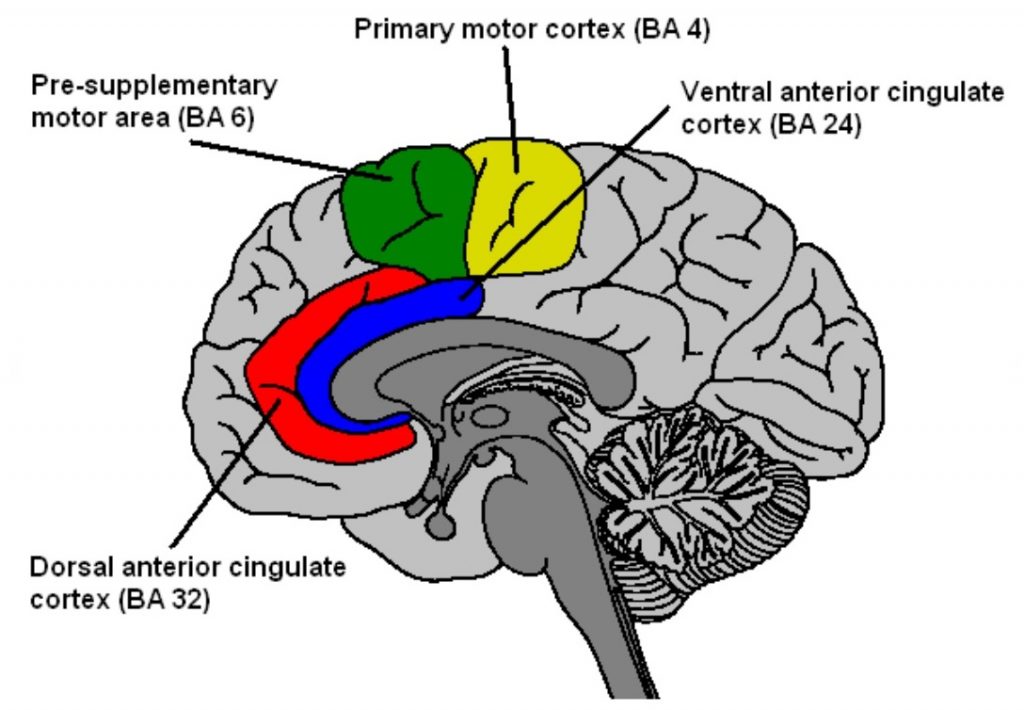
Image: Millan, Jose del R. (2007). Error-related EEG potentials in brain-computer interfaces.
They are thought to be the last areas affected by the neuropathology of dementia, which may explain why people with dementia respond to music even when they already exhibit signs of significant cognitive decline.
https://www.ncbi.nlm.nih.gov/pubmed/19214750
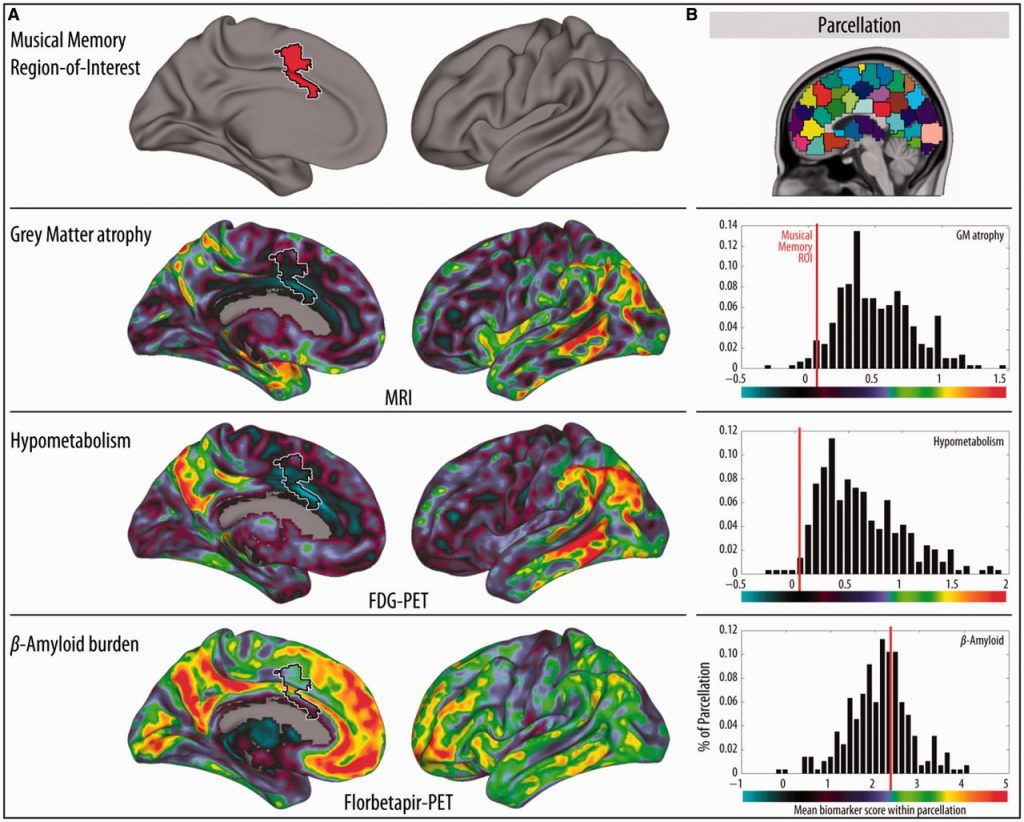
Image: Max Planck Institute for Human and Cognitive Brain Sciences
Not just music…
In fact, the creative arts in general play an important role in many aspects of dementia.
- Engagement with intellectual, social, physical and creative activities is associated with slower cognitive decline in older adults.
- Participation in the arts may delay onset and reduce severity of dementia, as well as improving quality of life for those living with dementia and their carers.
- Reflecting the health inequalities that exist throughout society, older people living in more deprived areas tend to develop dementia earlier and die from it younger than those living in more affluent areas.
In July 2017 an inquiry report was produced by The All-Party Parliamentary Group on Arts, Health and Wellbeing (APPGAHW). They strongly advised NHS England to include the arts in post-diagnostic, person-centred support for people with dementia.
Very long (150 pages or so) but an interesting read to dip in and out of.
https://www.culturehealthandwellbeing.org.uk/appg-inquiry/
Music for Dementia 2020 is a national campaign to help make music available for everyone living with dementia. In other words, we want to get music into the ears and lives of people living with dementia because we know music is transformative for them.
Music for Dementia 2020 was founded by The Utley Foundation, in response to the publication of the International Longevity Centre-UK’s Commission Report into Dementia and Music.
The report clarifies some of the gaps and needs regarding music services and powerfully strengthens the case for bringing music for dementia further into the public forum so that this vital work can grow.
The Utley Foundation is a private family charitable Trust, founded in 2014 by Neil and Nicky Utley, both passionate music lovers and musicians.
Since its inception, the foundation has been supporting and championing the use of music and music therapy to improve the quality of life for people living with dementia.
In September 2019, we launched the Musical Map for Dementia – an online directory to find music offers / services for people living with dementia across the country.
How do we know music works? We have an evidence base which comprises all types of data – real world to clinical trials.
Importance of personalised music:
- Music should be specifically tailored to the choices and preferences of individuals – these preferences can be expressed by people whose verbal skills have declined or are no longer available.
- Personalised music helps with seeing a person for who they are, beyond their dementia. Their connection with music comes to the fore and you see their relationship with that music come to life.
- Personalised music meets the principles of person centred care
- Music is all about people and relationships and so too is person centred care – this is one of the reasons music can be so effective.
- Personalised music is all about the right music, at the right time, in the right way, by the right person – the Musical Menu of Choice
- Benefits of personalised musical care extend beyond the person living with dementia, positive impact for carers (those around the PLWD) and the environments, the places and spaces that people are in.
- There is some evidence that retaining memory for music enjoyed between the ages of 10 and 30 is much more enduring.
- Music can be integrated into care plans throughout the dementia journey – Musical Dementia Pathway (to be published in April)
https://www.england.nhs.uk/blog/music-and-dementia-a-powerful-connector/
Music therapy
Music therapy is the use of music (improvised, live, interactive, recorded) to meet someone’s unique and personal needs.
These could be psychological, emotional, social, physical, cognitive or spiritual needs.
As we all have our own unique relationships with music, this can become an alternative means of communication when words are too much, not enough or no longer available due to illness, injury or disability.
Music is a powerful connector, it connects us to ourselves, those around us and the world around us, and in doing so helps to support and maintain relationships.
Central to how music therapy works is the therapeutic relationship that is established and developed between therapist and client, through engagement in live musical interaction and play.
A wide range of musical styles and instruments can be used, including the voice, and the music is often improvised. Using music in this way enables clients to create their own unique musical language in which to explore and connect with the world and express themselves.
Music therapists draw upon the innate qualities of music to support people of all ages from helping newborn babies to develop healthy bonds with their parents, to offering sensitive and compassionate palliative care at the end of life.
It can help to develop and facilitate communication skills, improve self-confidence and independence, enhance self-awareness and awareness of others, improve concentration and attention skills.
Music can be a social process engaged in with others and it can also provide the sanctuary of a more private experience. Depending on the individual needs of the client, music therapists offer individual or group music therapy sessions.
Here are a few examples of programmes that exist around the UK with the aim of bringing music to people with dementia:
Playlist for Life is a charity founded in 2013 by Sally Magnusson (a writer and broadcaster) after the death of her mother, Mamie, who had dementia.
Their practice is based on something called the Gerdner Protocol, developed at Stanford university, which is a guideline for using individualised music for people with dementia.
They promote the use of therapeutic scheduling – timing listening around certain activities (e.g. difficult tasks, spending time together, meeting new people).
This links to the idea of individualised music – depending on availability of musicians, equipment etc, this might be hard to achieve with live music. Tastes are going to change in coming years (more people liking louder, wilder and more electronic music).
Wishing Well – Music in Healthcare
Based in Sussex, Wishing Well brings live music to a range of healthcare settings with the aim of supporting wellbeing through a shared musical experience.
Their website has lots of wonderful videos of the team in action!
http://wishingwellmusic.org.uk/
Singing for the Brain: started in 2003 by the Alzheimer’s Society, it is a standardised service that follows a specific model across the UK. Sessions involve a musician, people with dementia, and their care-givers. They start with physical and vocal warm-up exercises, then move on to a themed singing session (i.e. the weather, travel) with some well-known songs and some new ones.
The programme has been seen to aid communication by strengthening neural pathways to the vocal and breathing mechanisms.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5089222/
It has also been the subject of a short film and has featured in a Radio 4 documentary.
https://www.bbc.co.uk/programmes/b01cjwtn
Alice spoke to Shreena Unadkat, a clinical psychologist, about her research on group singing for couples where one partner has a diagnosis of dementia.
Here is a link to her work:
https://www.ncbi.nlm.nih.gov/pubmed/26783138
And here is a video of the fabulous project at the Dulwich Picture Gallery, which we discussed in the interview:
Curriculum Mapping
NHS Knowledge Skills Framework
- Core 1 Level 3
- Core 2 Level 2
- Core 4 Level 1
- HWB1 Level 1
- HWB4 Level 3
Foundation Programme
- Sec 1:2 Patient centred care
- Sec 1:4 Self directed learning
- Sec 2:6 Comm. patients/ relatives
- Sec 3:10 Support for pts
GPVTS
- 3.05 Practising holistically and promoting health
- 3.05 Maintaining performance, learning and teaching
Core Medical Training
- Health promotion and public health
- Factors affecting health
- Other Important Presentations
- Aggressive / Disturbed Behaviour
- Geriatric Medicine
- MDT assessment
- Dementia
Internal Medicine Stage 1
- Generic CIPs – Category 1:1
- Learning & teaching
- Generic CIPs – Category 2:3
- Communicate with patients
- Barriers to communication
- Generic CIPs – Category 3:4
- Share good practice
- Generic CIPs – Category 4:5
- Role of evidence in practice
- Dementias
- Aggressive or disturbed behaviour
Geriatric Medicine Specialty Training
- Health promotion and public health
- Factors affecting health
- 29. Diagnosis and Management of Chronic Disease and Disability
- Influences of environment, culture and behaviour on access to healthcare and health outcomes
- 33. Dementia
- 49. Dementia and Psychogeriatric Services




